The HSE, and health care access more generally in Ireland, has never been under such scrutiny as has been the case in recent times. From the handling of the pandemic to the chaos witnessed during last year’s cyber attack, we now face recent revelations about utter confusion in the handling of funds and a recruitment crisis, exposed in leaked tapes published by the Business Post.
HSE CEO Paul Reid also admitted in a recent News Talk interview how, particularly recruitment issues, were “not going to be solved in one year.”
It is reasonable to assume that addressing structural dysfunctions in health services will take time, but we often forget the real impacts, and often irreversible damages on our most vulnerable members of society, caused merely by the passage of time. This applies especially to the treatment of complex conditions requiring a multi-disciplinary approach.
A most striking example is the effects on those children awaiting treatment for Spina Bifida/Hydrocephalus, and their parents.
We recently spoke to Amanda Coughlan Santry, the co-founder of the parent-led advocacy group Spina Bifida & Hydrocephalus Paediatric Advocacy Group, which has been active since 2017. It raises awareness around the lack of access to care for children affected by the condition, and actively engages with the institutions to address what seems one of the worst failings by the State in contemporary Ireland.
Amanda, along with other parents Una Keightley, Stefania Opinto, and Orlaith Maher Lalor, joined us for an in-depth interview which we hope can draw further attention to the current situation.
The group have recently launched a website www.sbhpag.com in which sixty-nine children’s stories are presented. Here one can discover the scale of the challenges surrounding their access to treatment.
We heard of children being left on waiting lists for surgeries for over a year for treatments, which in other European countries are urgently attended to. There have been years of complaints, which went for the most the most part unanswered and, most distressingly, in the last few months, parents of children in pain, have felt compelled to refuse to leave A&Es for days on end until their children were treated.
Reflecing on his long experience, whisteblower Chay Bowes concludes the Irish health system perpetuates dysfunction to the benefit of a private systemhttps://t.co/n0qDKuPcqv@BowesChay @broadsheet_ie @VillageMagIRE @caulmick @DrMarkMurphy @health_irish @RoryHearne @vincentbrowne
— CassandraVoices (@VoicesCassandra) November 16, 2021
Daniele: Can you tell us more about this condition?
Amanda: Spina Bifida is described as one of the most complex conditions compatible with life; a baby’s spine and spinal cord does not develop properly in the womb, causing a gap in the spine. Spina bifida is a type of neural tube defect. The neural tube is the structure that eventually develops into the baby’s brain and spinal cord.
Most people with spina bifida can have surgery to close the opening in the spine. But the nervous system will usually already have been damaged, which can lead to problems such as weakness or total paralysis of the legs, Urological, Bowel and Renal issues.
Many babies will be born with or develop hydrocephalus which is a build-up of fluid on the brain. This requires a V.P or a shunt to drain the excess fluid from the brain into the abdomen or the heart.
There are about approximately 550 children under 18 living with Sb/Hydro in Ireland. Ireland has one of the highest rates of neural tube/SB birth rates in the developed world.
Daniele: Can I ask you for a little bit of context to give an idea of the extent of the services needed?. What are the types of care that your children need?
Amanda: Our children need proactive care and what they are receiving is often reactive care via emergency intervention. This is often too late and results in long term damage and loss of function. These children need timely access to care particularly in relation to Orthopaedics, Urology, Ophthalmology, Neuropsychology and Neurosurgery.
Daniele: How are these types of care being delivered in Ireland and is the capacity in the health service enough to address the scale of the problem in Ireland?
Amanda: Currently the care in Ireland is sporadic, chaotic, under-funded & under-resourced. Some children have access to a Multidisciplinary Spina Bifida Clinic, others do not. There is no clear pathway of care for children living with Hydrocephalus alone. An annual MDT SB clinic is international best practice. We estimate 85% of SB children are not receiving this and the percentage is higher in children born prior to 2009.
Daniele: I gather that the waiting times are causing actual daily pain and suffering. If someone breaks a bone or a dislocation, he gets treated in a fairly short time. How’s that different from the pain that your children suffer? And what happens if you go to the A&E?
Amanda: I know of a child that received her surgery last month because the mother took the drastic measure of taking her daughter to accident and emergency and refusing to leave. She dug her heels in the A&E in Temple Street, until she was admitted. And once she was admitted sat for two and a half weeks before the child had her surgery.
In that process, the CEO of the National Children’s Hospital Group, Joe Gannon, subsequently wrote to one of the politicians in government who had been trying to fight for this child’s case, and told the politician that she was currently an inpatient and that she was going to have her surgery on the 17th of January.
He made it sound that it was a planned admission and that she had been given a date and they had come in.
Actually what happened is that the mother refused to leave until her daughter’s medical needs were met and also the child did not have her surgery until a week later. The mother is very grateful to all the doctors involved as they all told her that she was doing the right thing not to leave and were very supportive. She was supported in that sense by us as well but she should have never had to take such a drastic step.
We’ve had another number of families that have had to do this since last September.
Another mother went in on a Saturday with her son, who had dislocated hips for four years, the child is six, and she refused to leave until they were admitted. And once they were admitted, they couldn’t see the surgeon because he wasn’t there. They refused to leave and sat there for 10 days until their child had the surgery.
Daniele: How did your organisation come into being?
Amanda: We’re all parents of children with spina bifida or hydrocephalus that came together to advocate for better services for children, under the age of 18, living with Spina Bifida/Hydrocephalus in Ireland.
Our group was formed in 2017 and have been trying to work in a proactive and collaborative manner with all relevant stakeholders since then.
My own son was one of the children failed, he sat on a waiting list from 2014 to 2016, and by the time he’d seen a spinal surgeon in 2016, we were told it’s too late.
So my son lives with inoperable scoliosis and he cannot be helped by this campaign or anything else but I wanted to do something to stop this from happening to other children. Una Keightley was one of the very first to come on board when we formally launched the paediatric advocacy group.
Daniele: Una Keightley, what pushed you to take a more proactive role in dealing with the issue?
Una: I suppose it did become quite apparent that no matter how many letters you wrote, like what Amanda had said, the situation didn’t improved. She wrote to everyone, she had highlighted it. And it just really concerned me. And I’m a health care professional. I’m a radiation therapist and it was just unbelievable to me that this was going on. And I suppose at that stage my child was younger when we came together. Once we talked to more and more parents we realized that people were actually lodging complains but they were going nowhere.
So we started to proactively inform the powers that be and Children Health Ireland asking them to do something about it.
Amanda: There is a cohort of children born prior to 2009 who had no access at all to this to the Spina Bifida team in Temple Street Hospital because there was no urologist on that team. So it was decided it was safer to leave the children in Crumlin Hospital and move them at a later stage. A urologist didn’t come onto the team at Temple Street until 2014, and the children were never moved. So a lot of our children were receiving inadequate services are no service at all.
We highlighted this problem in 2018 with the CHI board. In that meeting, they asked us, our advocacy group, to go back to the families and identify whether they felt that they weren’t receiving a timely access to services or any services at all. So we did, which was a big job being undertaken because we’re volunteers.
There was also a cohort of families who thought that their children were being treated but many other that did not.
Una: In the beginning of 2019, we gave Children’s Health Ireland a list of 133 families and children who felt that they weren’t receiving a proper service. There was then so many e-mails back and forth between Amanda and CHI. We asked them: When can we meet? What are we going to do about this? And the answers were like: “We’re verifying the list.” “We are analysing the list.”
We have screen shots of these emails.
That one way communication continued for probably 18 months until, after March 2020 they just ignored us.
Entering 2021 we felt we had to do something but, on top of that, I need to say that I suppose a lot of parents were fearful. If they talk out, maybe the care standard that would be provided to their child would be diminished. Now, I wouldn’t have that fear, and I don’t think any of us would.
It was especially after Professor McCormack and Prof Connor Green had presented before the Oireachtas health committee in November 2021 that things were very desperate, that it became blatantly obvious that it was a systemic failure for our children.
It was then when we decided to publish online our children stories. Which is something that distressed us greatly but we felt we were left with no choice.
We had requested to meet the Minister ever since he took up office. He wouldn’t meet us. The Minister for Children wouldn’t meet us. The Minister for Disability wouldn’t meet us. Nobody would take up and highlight what was happening to these children. So the parents as a group decided that we were going to have to do something fairly drastic to get their attention. So that’s what we did.
Daniele: I have noticed an increase in media attention to the issue in 2021, also thanks to your campaigning. Are you hopeful that increased scrutiny could move things in the right direction?
Amanda: Yes, people now view our children as the vibrant individuals they are as opposed to a number on a list or a medically complex child that is unrelatable. The support received initially from media, County Councils, and local representatives across all 26 counties has been immense. This has stemmed from the proactive and
drastic measures taken by the Paediatric Advocacy Group and the families to highlight the failures in care for their beloved children.
People have been shocked by the current state of medical neglect that has
been inflicted by the Irish state on our children. They are not willing to allow a further generation of children to be failed and to turn a blind eye to the historical neglect that has been allowed to happen.
Daniele: After years of campaigning, countless letters to TDs and local councillors, you have finally met with Minister Donnelly along with Spina Bifida Hydrocephalus Ireland and other stake holders last February in relation to the abnormal waiting times that are now in place for paediatric orthopaedic treatments. Plans have been presented and funding – as much €19 million that the HSE made available to CHI –, albeit with little information on the specific break down. The Minister also set some clear goals, including to limit the waiting time to four months at first with the aim for this to be reduced to zero, and to provide a number of additional treatments. What’s the reaction from you and your organization to these pledges?
Amanda: There aren’t many details released yet, and there is still a draft in formation. What they told us is that they have ring fenced €19 million for children with spina bifida, but also to children with scoliosis.
They have also said that clinically no child should wait for more than four months for surgery. So that is very ambitious and while we’re glad about these pledges, we’re not blindly trusting. There’ve been promises made before not only to us, but to the scoliosis advocacy groups as well. So yes, the funding is great, but we need to see that the funding is going to make a real difference in these children’s lives.
One of the government target is to “treat an additional 107 Spina Bifida cases” but we don’t know how they come up with that particular number. There is no database within CHI of how many children are living with the condition. So how do you come up with a number if you don’t know how many children you’re treating, do you know? So we’re a little bit dubious about it and we don’t want to be tied to that number. What we want is to fund and to reach as many children as possible.
Daniele: Did the Minister agree to regularly update your organisation while they endeavour to deliver these pledges?
Amanda: We do have a commitment from Stephen Donnelly and Children Health Ireland, to regularly engage with us and we do now have a contact with one of the Minister’s special advisers. So if an issue comes up or we want to speak to Donnelly, all I have to do is give the special adviser a ring and he will relay any information and if need be we speak to the Minister directly. So that’s the promise we have. So we are we’re optimistic and he seemed very genuine when we spoke to him. But don’t intend to take the pressure off until this gets sorted. We intend to stay very, very focused.
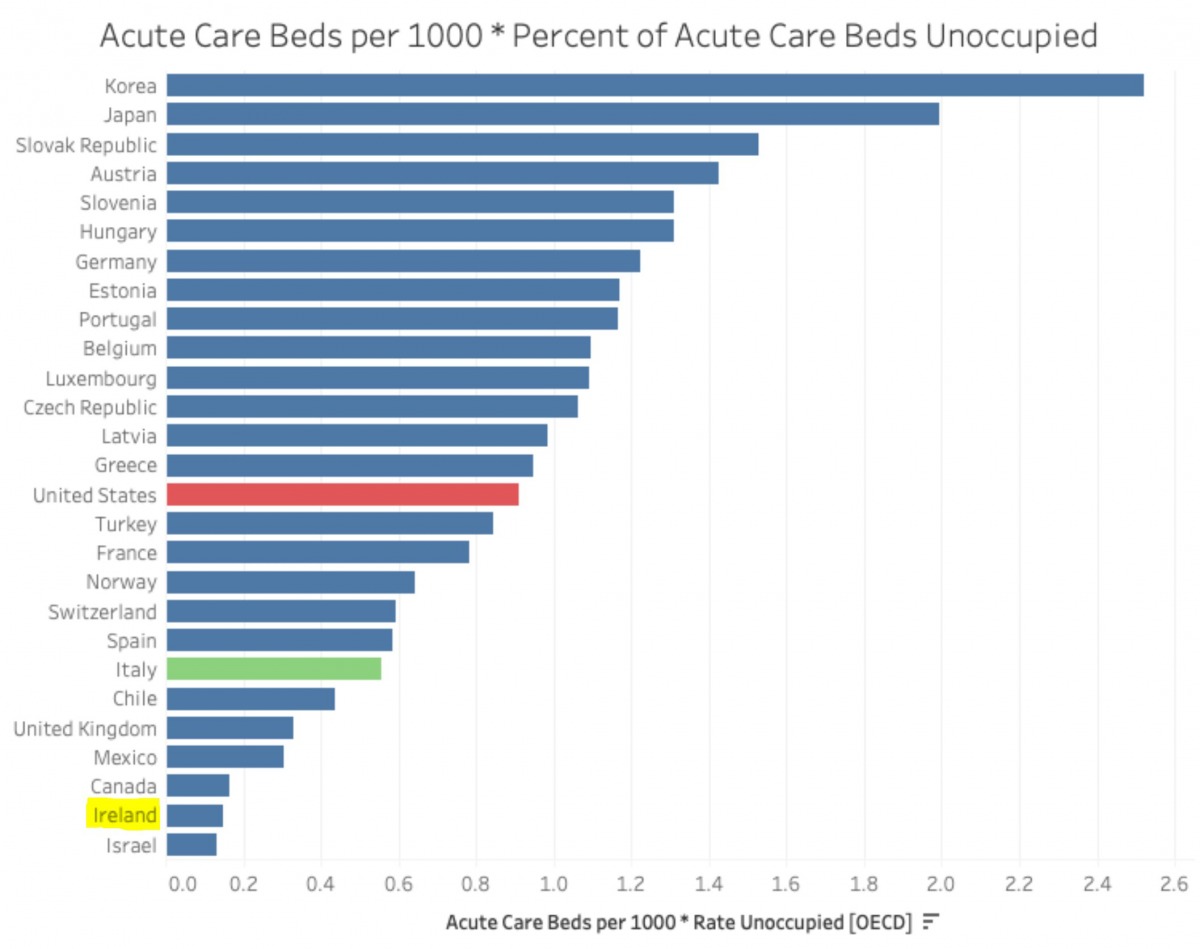
Daniele: Are there any kind of league tables or other international comparisons that can be drawn on?
Una: It would be difficult because we have such a high rate compared to a lot of the world. What we do know is that in Ireland it is not the expertise that is missing but proper funding and organization. Cases are picked up in pregnancy here more than they are in other countries, probably because the stenographers are looking for them due to the high incidence.
Daniele: What kind of challenges are you dealing with as mothers and what are the support needed for families at large?
Stefania: My daughter’s name is Aurora and she’s just turned three. From her birth in February 2019 until August 2019 she was in hospital as she was born with Hydrocephalus.
I found out about that on my 26 week scan here in Ireland and to be honest with you I didn’t know what it meant so I had to do my own research. They didn’t explain to me exactly what it was. So I had to go back to Italy, and I went to the hospital in Genoa to try to get different opinions.
Once she was born, here in Ireland, she needed to go straight for surgery because there was too much pressure on the brain because of these fluids. And so we got transferred first to Temple Street, and after two weeks to Crumlin.
I just want to clarify that doctors and nurses were fantastic to me, to my husband and to Aurora. She wouldn’t be here if the surgery hadn’t been successful.
Having said that there definitely gaps in the communication between the two hospitals. They were relying on the parents to get the information, which is not ideal because I’m not a doctor and that created frustrations and fears.
When our daughter was released from hospital we were pretty much left to our own devices. She had just one appointment in Temple Street during her first year. And after that, I’ve been told that I needed to wait another year. Initially I thought that such a long time between visits was just because she’s doing well but It’s not the case. There was lots of information that I had to get elsewhere, and not from the professionals. In terms of psychological support for parents, we were very much left on our own. So you either cope and become resilient or probably you’re not going to make it mentally. I’m grateful I found this group and that these ladies became my source of knowledge.
Una: In terms of the financial support as well, like. Many of us received no financial support because our husbands or partners were too high earning So although your child has very high medical care needs – you could have a child who’s on oxygen 24 hours a day – you won’t get one penny from the government.
Orlaith: In my case, my daughter is 20. We were under a multi-disciplinary team but with only three consultants in it. And after 2008, Crumlin finished up its spina bifida clinic. We then ended up being spread over four hospitals which don’t share files. So as Silvana said earlier, it is up to the parent to bridge the gap.
When she was born she was very ill for the first four and a half months. We lived in the hospital paying for parental accommodation.
I had my dream job. I worked in the Irish Times and I was part of the first team to ever bring in supplements into a broadsheet newspaper. I went on carer’s leave and eventually ended up leaving my job.
There was no support for children with hydrocephalus. It’s not considered an intellectual disability. So, you know, you’re very much left on your own. My husband had a good job. I’ve never received Carer’s allowance after the first four or five months that we spent in hospital with her.
When my daughter was seven they took away her medical card. In this country, when the medical card is taken away, your medical hardship scheme is directly attached. So a lot of the equipment you need you have to pay for it yourself.
At nine she had three failed shunts, and two brain bleeds ending up spending nearly four months in Beaumont Hospital. I had to pay for my parking every day, for my accommodation and my food. Thousands of euros. I can’t claim back anything on that. And we still had to pay our bills and our mortgage.
There’s a lot of stress around dealing with the child that’s sick and sure, you’re not failing your special child as you’re doing the best you can. On top of that, you’re fighting for everything. You’re fighting for therapy, you’re fighting for access to care, you’re fighting for basic things like my daughter’s incontinence and the allocation of nappies. It compounds into a heavy psychological weight. It’s not the disability alone, it’s the lack of support; the lack of access to timely care and that constant heavy worry all the time. They need help. I can’t get them help. I can’t force my appointments. I can’t force the consultant to do this or that. My daughter has now aged out of paediatrics and there’s no transition pathway. So now my job is going to my GP all the time. She had her first orthopaedic appointment in five years two weeks ago, and that took 16 adult consultants to refuse her before we got that orthopaedic consultant. So there’s lots of stress on you all the time.
Here in Ireland, we have great nurses, we have great doctors, and I wouldn’t made it without them, but they’re not resourced and there doesn’t seem to be a willingness to accept we have such a high rate of these cases and that it needs to be invested in.
Amanda: In the space of 18 months, my son went from needing care to becoming completely inoperable. For the first couple of years. He had a lot of appointments. Then it that stopped.
My relationship with my partner deteriorated and broke down, very early on due to the stress and the strain of trying to care for a very medically vulnerable child. I suddenly became a single working mother with two children, one with massive medical need and not financially supported by the state. I worked full time, paid a huge amount of rent. I’ve subsequently remarried and have gone on to have other children. Thankfully, my husband came into this with an open eyes.
We wouldn’t change our children, what we would do and what we want to do is to change the services for them. They can become independent within their capabilities, and live their lives to the fullest without the need to be in pain or to have their parents struggling and fighting for services.
https://twitter.com/BillyRalph/status/1458052402372923392
Daniele: Over the last two years of pandemic, and with the HSE coming under cyberattack, your stress levels must have been almost unbearable. Having said that it is quite evident that these dysfunctions were there prior to these. How have you coped?
Amanda: I’ve spoken to numerous families about this and we acknowledge that the pandemic and the cyber-attack happened, It was very scary and nobody had to protect our children more than we did.
But what happened in the pandemic? The small amount of services and extra curriculum activities that our children were receiving stopped.
Physiotherapists, occupational therapists were all redirected to COVID services and we understand the need for that. But there was also a huge recruitment drive by the HSE up thousands of health care professionals, like myself were ready to help but weren’t called up.
We know now that during the pandemic, orthopaedics accident where less frequent so why weren’t our children’s needs met within this timeframe when obviously there was the space to meet them given the cessation of extracurricular activities?
As parents, we would call the pandemic and the cyberattack, the new great excuse for not giving us an appointment.
Our children didn’t just freeze their conditions for two years or three years. You know, they continue to deteriorate.
Stefania: My daughter Aurora, she has malformation of her ribs and she has never seen an orthopaedic surgeon in the last 3 years.
It’s not that the doctors aren’t aware. Her Cardiologist took her case to his heart and did his best to advocate within Crumlin Children Hospital and he really fought for me but it’s not his job to organize a better multidisciplinary care structure.
Daniele: That would be the job of the administration I presume. To conclude, how do you think Irish society perceives disability and how can awareness be promoted?
Amanda: Irish people generally would be viewed as very laid back and positive.
Therefore, there is an element that “disability cannot happen to me!”. It is only with an ageing population, inaccessible public transport, inaccessible housing, and educational facilities that the message is relayed to the ordinary person about how vast the inequality is between the non-disabled & disabled communities in Ireland.
Over the last few decades Ireland has become a more diverse nation. Our children are exposed to more languages, ethnicity and religions than has ever been present on this island.
These are the children of a new and inclusive Éire and as such, they do not have the same prejudices and intolerances as those who have gone before them. Our children living with disabilities are accepted by their peers and integrated more within society.
It is deeply distressing for us that the relevant stakeholders within government and the Irish health care system, have not adopted the same attitude and continue to treat our children like second class citizens.